Home » Posts tagged 'New York City'
Tag Archives: New York City
Back to the Lab with Dr. Jason Rauceo

John Jay College, along with CUNY schools across the city, are moving toward the resumption of on-campus life. Classes are attended in-person, events are being planned, and professors and students alike are headed back into the laboratory. I talked to one of John Jay’s professors in the Department of Sciences, Dr. Jason Rauceo, to find out what it’s been like closing down and reopening his lab.
Dr. Rauceo is an Associate Professor of Biology whose research focuses on the major fungal pathogen Candida albicans. He is also the Director of the Cell and Molecular Biology major at John Jay. In 2021, Dr. Rauceo received a four-year grant from the National Institutes of Health to study the role of the mitochondrion in C. albicans’ ability to infect hosts and cause disease.
What was it like to get back to lab work after a significant time away during the early part of the pandemic? Did you have to change any protocols or make adjustments to your operating procedures?
Right before CUNY closed in March 2020, I shut the lab down with the expectation that I would not return for 6-12 months. I returned to campus in September 2020, and the major challenge was reopening the lab myself. Students were not allowed on campus, and I needed to calibrate several instruments that I had limited experience operating. Fortunately, my students were available via Zoom and FaceTime for assistance.
What does a typical day in the lab look like, if there is such a thing?
The day usually begins with a short one-to-one meeting with whomever is scheduled to perform an experiment, in which we mainly discuss logistics. Throughout the day, I periodically check in to assist and address any experimental issues if needed. At the end of the day, I inspect the lab to make sure that workspaces are cleaned, all reagents and supplies are properly stored, and all students have left the lab.

What function do students play in your lab?
Students perform the hands-on experimentation and data analysis, and are responsible for general lab maintenance. They also contribute to the development of their projects, which must be directly related to the lab agenda—in this case, C. albicans biology. Students may propose their own experiments for approval after approximately 1.5 to 2 years of experience in the lab.
You place a lot of emphasis on experiential-based learning. What does that mean in practice for your students?
I allow students to test their own hypotheses when safety and costs are not an issue. Also, I allow students to make their own errors during initial training exercises. I found that this approach in lab research builds confidence.
Generally, in the early stages of a new project, a significant amount of time is devoted to optimizing protocols to meet our objectives. During this “optimization phase” of the research, there is an extensive level of troubleshooting required, and a high level of error and ambiguity is observed. I found that a major payoff of experiential-based learning and training is that students propose unique approaches to addressing experimental obstacles.
Your study of SPFH (Stomatin, Prohibitin, Flotillin, HflK/HflC) proteins’ role in mitochondrial function in Candida albicans is being funded by the NIH. It seems that there are some exciting implications for developing antifungal treatments—can you tell me about that?
SPFH proteins are widely conserved in nature and are found in most living organisms. These proteins are important for major biological processes including, but not limited to, respiration, transport, and communication. Candida albicans is a fungus that resides in all humans on mucosal surfaces such as the mouth and gastrointestinal tract in a harmless state. However, changes in our immunity sometimes cause C. albicans infections. Immunocompromised individuals are highly susceptible to C. albicans infections.
Currently, the function of SPFH proteins is limited in C. albicans. We were the first research group to demonstrate that SPFH proteins are required when C. albicans is challenged with environmental stress. Our current proposal seeks to define the molecular function of SPFH proteins. We are collaborating with several prominent research groups in fungal biology and medicinal chemistry to determine the function of the SPFH proteins in mitochondrial function.
One of our project aims is to understand the effects of treating C. albicans with natural compounds that target SPFH proteins. Our initial findings are promising and may be useful in developing novel antifungal strategies.
The NIH award provided me with the funds to expand my lab operations, and I’ve recruited three new undergraduate students; therefore, I will be spending much of the next semester in student training and performing experiments.
Sewage and the Science of Public Health – Dr. Shu-Yuan Cheng and Dr. Marta Concheiro-Guisan Track Wastewater Contaminants

Wastewater is a topic that the average New Yorker doesn’t think about often, but perhaps we should. Sewage and run-off, over a billion gallons of which are treated every single day in New York City by 14 wastewater resource recovery facilities, are a valuable resource for scientists.
Wastewater sampling has been a useful tool for public health researchers tracking the COVID-19 pandemic over the last two years. The Centers for Disease Control (CDC) launched the National Wastewater Surveillance System in September 2020 as a means of tracking virus spread and community prevalence. Viral genetic material is transmitted in fecal matter to the sewers and waste treatment plants, where researchers can take samples. Their work can serve as an early warning of community spread, track variants, and inform public health strategies for responding to the virus. Even better, wastewater surveillance doesn’t require individuals to seek out healthcare in order to capture information, meaning that the resulting data can include people who may be asymptomatic, who have taken home tests, or who have not been tested at all.
Wastewater data have figured prominently in several interesting COVID-19 stories recently in the news. In January 2022 the CDC reported that mutations associated with the Omicron variant showed up in New York City wastewater in November 2021, before the variant was officially reported in South Africa and at least a week before the first U.S. case was identified via clinical testing, suggesting that Omicron was likely circulating in communities before cases could be officially confirmed. And The New York Times recently reported on mysterious fragments of viral RNA with novel mutations detected in NYC wastewater, which are stumping researchers. They haven’t been able to pin down where these fragments are coming from, nor why these mutations have not shown up in clinical testing of human or animal populations in the city.

Two John Jay College researchers, Dr. Shu-Yuan Cheng and Dr. Marta Concheiro-Guisan, are also big proponents of wastewater sampling studies as a public health tool. Their own research, published in 2019, tracked drug use over one year in New York City, using one-time grab samples to test for levels of cocaine, nicotine, cannabis, opioids, and amphetamines in the sewage. Now, the scientists are collaborating with non-profits that test the health of the city’s waterways, trying to correlate levels of pharmaceuticals in our rivers with the amount of harmful bacteria.
To Dr. Cheng and Dr. Concheiro-Guisan, wastewater analysis’s great strength lies in early warning and early intervention. “It’s a great tool for prediction, for public health, crime fighting, and disease [prevention] purposes,” says Dr. Cheng. “The official report is often too late, but if you can do an early intervention, find the issue and start addressing it, there’s a lot you can do.”
“We looked at wastewater because we saw the utility,” says Dr. Concheiro-Guisan. “This is a different application [than viral tracking] but with the same thought: that what we eliminate from our bodies tells you a lot about your population.”
However, the United States is late to the game. Though the CDC has had results with its national COVID-19 tracking program, both researchers lament the lack of a centralized American body to apply this research to other public health applications. They’d like to see the U.S. follow the example set in European countries, China, Australia, and increasingly in South America, where governments have applied wastewater sampling to create campaigns warning their citizens about novel psychoactives, catch drug manufacturers, and more.
“It’s a very important public health tool that is showing results,” says Dr. Concheiro-Guisan. “If you start in the biggest city in the country, if you start in New York, then others will follow.”
 Dr. Shu-Yuan Cheng is an Associate Professor and Chair of John Jay’s Department of Sciences. Her research is in the areas of toxicology and forensic pharmacology, including the roles that environmental toxins play in neurodegenerative diseases, identifying the target genes and signaling pathways affected by environmental toxins, and investigating pharmacological mechanisms of anti-cancer medications.
Dr. Shu-Yuan Cheng is an Associate Professor and Chair of John Jay’s Department of Sciences. Her research is in the areas of toxicology and forensic pharmacology, including the roles that environmental toxins play in neurodegenerative diseases, identifying the target genes and signaling pathways affected by environmental toxins, and investigating pharmacological mechanisms of anti-cancer medications.
 Dr. Marta Concheiro-Guisan is Assistant Professor of Forensic Toxicology in John Jay’s Department of Sciences. Her research focuses on the development and validation of analytical methods by gas and liquid chromatography tandem mass spectrometry and their application to different specimens, the detection of drug exposure during pregnancy, and the toxicological study of new psychoactive substances.
Dr. Marta Concheiro-Guisan is Assistant Professor of Forensic Toxicology in John Jay’s Department of Sciences. Her research focuses on the development and validation of analytical methods by gas and liquid chromatography tandem mass spectrometry and their application to different specimens, the detection of drug exposure during pregnancy, and the toxicological study of new psychoactive substances.
Frank Pezzella Wants Increased Accountability on Hate Crime Reporting
During the chaotic years of the Trump Administration, the United States experienced a rise in hate crimes. This increase has been confirmed by FBI data collection, media reporting, and independent scholarship. According to Dr. Frank Pezzella, an Associate Professor of Criminal Justice at John Jay College and a scholar of hate crimes, four out of the past five years, from 2015 to 2019, have seen consecutive increases in hate crime offending in this country, something he says is new. Nine of the ten largest American cities had the most dramatic increases in hate crimes – including New York City.
Hate crimes, or bias crimes, are strictly defined by the FBI. The organization sets out 14 indicators that must be present for a criminal offense to be classified as a hate or bias crime, that provide objective evidence that the crime was motivated by bias. But according to Dr. Pezzella, the evidence to meet those criteria isn’t always clear. Not every hate crime is as flagrant as the Pulse nightclub shooting in 2016 or the 2018 attack on Pittsburgh’s Tree of Life Synagogue. To establish a hate crime was committed, first responding police officers must look for evidence of bias motivation – what Pezzella calls an “elevated mens rea” requirement. But bias can only be committed against legally protected categories, like race and ethnicity, sexual or gender orientation, disability, or religion, which vary from state to state. And the additional paperwork and procedural requirements that come with classifying an incident as a hate crime are, in his words, disincentivizing police reporting.
Undercounting Hate Crimes
 The result of these complications is rampant underreporting. In his new book, The Measurement of Hate Crimes in America, Dr. Pezzella looks at the reasons why hate crimes are so undercounted in the United States, and proposes some solutions for what law enforcement and policymakers can do to correct the issue. Since the enactment of the federal Hate Crimes Statistics Act in 1990, which required the Attorney General to collect data about hate crimes, the FBI has been fulfilling this mandate in the form of the Hate Crime Statistics Program, published annually as part of the Uniform Crime Report. According to Dr. Pezzella, since 1990 the UCR has reported an average of roughly 8,000 hate crimes per year; but victims, he says, report around 250,000 hate crimes per year. He attributes this substantial gap to a variety of factors including the evidentiary and procedural barriers noted above. In addition, only about 100,000 of these victimizations are ever reported to the police in the first place. And when victims do report, police departments are under no legal requirement to pass their findings on to the FBI.
The result of these complications is rampant underreporting. In his new book, The Measurement of Hate Crimes in America, Dr. Pezzella looks at the reasons why hate crimes are so undercounted in the United States, and proposes some solutions for what law enforcement and policymakers can do to correct the issue. Since the enactment of the federal Hate Crimes Statistics Act in 1990, which required the Attorney General to collect data about hate crimes, the FBI has been fulfilling this mandate in the form of the Hate Crime Statistics Program, published annually as part of the Uniform Crime Report. According to Dr. Pezzella, since 1990 the UCR has reported an average of roughly 8,000 hate crimes per year; but victims, he says, report around 250,000 hate crimes per year. He attributes this substantial gap to a variety of factors including the evidentiary and procedural barriers noted above. In addition, only about 100,000 of these victimizations are ever reported to the police in the first place. And when victims do report, police departments are under no legal requirement to pass their findings on to the FBI.
“Of the roughly 18,500 police departments, only maybe 75% participate in the Uniform Crime Report hate crime reporting program – note that it is voluntary,” says Pezzella. “So we don’t even know about hate crimes in 25% of precincts. And of the participating 75%, roughly 90% report zero hate crimes every year. So one of the reasons we wrote the book is that, either we don’t have hate crimes the way we think we do, or we have a systemic reporting problem.” It’s obvious which he believes is true.
The consequences of underreporting hate crimes are severe, Dr. Pezzella says. “To the extent that we underreport both the type and extent of victimization, it really does put a specific policy issue in front of us. We need to know who’s being affected, how they’re being affected, and the extent of the effect, in order to fashion remedies.” The only way to target treatment and services for the most vulnerable and likely victims is through accurate reporting.
Remedying Undercounting
In order to remedy undercounting and better target policy, Dr. Pezzella presents a number of recommendations in The Measurement of Hate Crimes in America. He calls for changes to take place within police departments, at the level of state and local politics, and in the criminal legal system. First, he suggests that every precinct have a written and clearly posted hate crime policy, and that every officer be trained to understand the rules for identifying bias crimes and the statutes governing them in their particular state. He would also like to see greater police-community engagement on this issue, with better tracking of non-criminal bias incidents – like seeing a swastika or other racist tag in the neighborhood – which Pezzella says often lead to violent bias crimes. He would especially like to see hate crime reporting made mandatory, with penalties or audits following a departmental report of zero bias crimes in a year.
Stepping out of police departments, Dr. Pezzella also calls for greater engagement from state and local politicians, who after all control the purse strings as well as set state legislation, but who are often hesitant to call attention to a problem with hate crimes in their district. Finally, he wants prosecutors’ offices to commit to seeking hate crime convictions, rather than settling for the easier task of convicting an offender for non-bias equivalents. With every actor across the board invested in tackling hate crimes and being transparent and proactive about applying best practices, offenders are put on notice that the community, including police, won’t allow these harmful crimes to continue.
Vicarious Victimization
Dr. Pezzella has been studying hate crimes since his graduate school years at SUNY-Albany, but he doesn’t feel he’s reached the end of this line of research. Going forward, he is interested in studying the deleterious and vicarious effects hate crimes can have on the victims’ communities. Because bias-motivated offenders target victims based on what they are rather than what they do, Dr. Pezzella says, there is a sense that anyone could become the next victim. This impersonal threat undermines societal ideals of trust and equality, and can even affect property values, as whole groups feel unsafe in certain areas and may be forced to relocate. Pezzella also mentions the psychological and emotional impacts of feeling under threat for simply being who and what you are. “When a victim goes home and says they were a victim of a hate crime, in what way does it impact the quality of life or sense of safety for secondary victims [i.e., the victim’s community]?” he asks. “What do they do? While we understand the direct impact, we know less about this vicarious impact, and how far it extends beyond the primary victim.”
He also has his eye on current events, especially the rise of domestic terrorism in the United States. Dr. Pezzella is concerned about the growing number of organized hate groups in recent years, and how emboldened they have been by rhetoric from the top levels of government. While many mass shootings have been categorized as domestic terrorism, Pezzella also sees evidence of bias that might categorize these events as hate crimes. If they are being left out of crucial counts that help to allocate resources and fight back against hate in this country, he wants to know.
 Dr. Frank Pezzella is an Associate Professor of Criminal Justice at John Jay College. His primary research focus is on the causes, correlates, and consequences of hate crimes victimizations. He also conducts research on issues that relate to race, crime and justice. In addition to his most recent book, he is also the author of Hate Crime Statutes: A Public Policy and Law Enforcement Dilemma, as well as numerous peer-reviewed articles.
Dr. Frank Pezzella is an Associate Professor of Criminal Justice at John Jay College. His primary research focus is on the causes, correlates, and consequences of hate crimes victimizations. He also conducts research on issues that relate to race, crime and justice. In addition to his most recent book, he is also the author of Hate Crime Statutes: A Public Policy and Law Enforcement Dilemma, as well as numerous peer-reviewed articles.
A Critical History of Incarceration in New York City

Dr. Jayne Mooney is an Associate Professor of Sociology at John Jay and a member of the doctoral faculty of Women’s Studies and Sociology at the CUNY Graduate Center. She is also a director and founding member of the Critical Social History Project (CSHP), a research initiative and part of John Jay’s Social Change and Transgressive Studies Project that draws on archival material to shed light on the history of incarceration in New York City.
The project began in 2015 with a conversation spurred by reporting on abuse, poor conditions, and a rash of tragedies at Rikers Island; how best, Mooney and colleagues wondered, to preserve the memories of those who had been affected by the infamous jail, including not only the incarcerated but also their friends and families, guards and educators? And so they began the “Other City” project, which forms the largest component of the CSHP. Informed by their research into the history of New York’s penitentiary system, Mooney’s working group is pointing out the problems inherent in Mayor Bill de Blasio’s administration’s proposal to close Rikers and open four new city jails.
“On the most basic level, what we’re showing is that the current proposals are reinventing the wheel. It’s the same thing that’s always happened. Closing an institution and setting it up again, you’re going to have the same problems, because you’re not getting to those deep-rooted, structural issues,” says Mooney.
Reinventing the Wheel

In a forthcoming article, “Rikers Island: The Failure of a ‘Model’ Penitentiary” due to be published in The Prison Journal in 2020, Mooney and her co-author, CUNY graduate student Jarrod Shanahan, go through the instructive failures of incarceration reform in New York City back to the 1735 construction of the Publick Workhouse and House of Correction. They argue that a lack of historical documentation has allowed policymakers to strategically “forget” the failures of past “model” or “state of the art” institutions, continually replacing old jails with new without a look at the larger issues that have led to waves of highly praised but ultimately unsuccessful penal reform.
Set against the backdrop of historical, social and political context, Rikers’ closure and the proposals to replace it look familiar. “All of these places opened in the spirit of optimism—everything was going to change. And then everything goes wrong, these institutions are denounced as embarrassments, and the decision is made to close them down and rebuild. Of course, that’s what’s been happening in the present moment,” Mooney says. She and her colleagues encourage the Mayor’s Office to look beyond the walls of the prison for new solutions to social problems faced by New York and, indeed, the United States.
(Read her December 2019 letter to The Guardian on the subject, “Rikers has failed like others before it, but the solution is not new jails.”)
Preserving Voices, Preserving Justice

Mooney’s challenge to the new proposals is grounded not only in her work in political social history, but also in her background as a critical criminologist. “There’s a very strong abolitionist line all the way through critical criminology,” she notes, which informs the way the Critical Social History Project has approached critiques of the plan to build new jails.
The CSHP isn’t only focused on documenting mass incarceration in NYC. As the Vice Chair of the American Society of Criminology’s Critical Criminology and Social Justice Division, as well as the archivist, Mooney has been accumulating archival information related to the division and the field’s history of activism. The CSHP’s Preserving Justice component, jointly directed by Mooney and Visiting Scholar Albert de la Tierra, has created an exhibition in the Sociology Department displaying some of the core critical criminology texts. It’s open to any students, faculty or staff who are interested in the history of the field and the work of its important thinkers.
Expanding Research Horizons
Mooney is proud to talk about her team of dedicated researchers, which includes both undergraduate and graduate students. With the help of their diverse experiences and interests, the Critical Social History Project is expanding its remit, from the history of Rikers Island to topics including the history of women’s incarceration, other New York carceral institutions including the Tombs and Sing-Sing, mental illness and incarceration, and more. Together, they are showing the persistence of the problems related to the history of mass incarceration, no matter where in history you begin your research—up to and including the present day.
 The Critical Social History Project is directed by Jayne Mooney and Albert de la Tierra. Other members are Sara Salman (Victoria University of Wellington), Nick Rodrigo, Jacqui Young, Susan Opotow and Louis Kontos, as well as John Jay students Camilla Broderick, Anna Giannicchi, Tayabi Bibi, Andressa Almeida, Marcela Jorge-Ventura, and Audrey Victor.
The Critical Social History Project is directed by Jayne Mooney and Albert de la Tierra. Other members are Sara Salman (Victoria University of Wellington), Nick Rodrigo, Jacqui Young, Susan Opotow and Louis Kontos, as well as John Jay students Camilla Broderick, Anna Giannicchi, Tayabi Bibi, Andressa Almeida, Marcela Jorge-Ventura, and Audrey Victor.
You can learn more by visiting the Critical and Social History Project’s website.
Podcasting at John Jay: Making Research Accessible
If you’re like us, you love podcasts enough that you’ve subscribed to more than you can listen to in a week of subway commutes. Podcasting, then called online radio, rose in popularity with the proliferation of mp3 players in the early 2000s. In tandem with other personal platforms like blogs, podcasts exemplified the “democratizing spirit” of the internet.
Today, they are big business. Since the release of Serial in 2014, podcasts have boomed. Monthly listeners have nearly doubled since 2014, from around 39 million Americans to an estimated 90 million. As the listening audience grows, quality improves, and bigger names get interested in the medium, advertisers are investing millions.
At John Jay, interest in podcasting has risen along with the medium’s growing potential. The college is home to a variety of podcasts, run by students, faculty and staff, on a rainbow of topics. For example, students in the English department work with Professor Christen Madrazo to write, produce, and edit Life Out Loud, which highlights the diverse voices and real stories of John Jay’s student body. We also have faculty working on podcasts hosted outside John Jay, podcasts run by research centers, and faculty and staff who produce their own shows, right here on campus.
We will introduce you to two homegrown John Jay podcasts that seek to translate scholarship into a form that everyone can understand. Meet Kathleen Collins, a Reference Librarian and Professor at John Jay College, and Nick Rodrigo, a CUNY Ph.D. candidate and John Jay College adjunct professor. While Kathleen is on her 38th episode of podcast Indoor Voices, and Nick has just released the first six episodes of They Are Just Deportees, both share the desire to take CUNY research out of the ivory tower and bring it to the community.
 Kathleen Collins has been producing Indoor Voices since the summer of 2017. She started the podcast as “a way to highlight the fascinating things going on around CUNY that might not be widely known. There are so many inhabitants in the CUNYverse doing incredibly interesting things… We like being able to provide a low-stakes, easy-to-share platform for people to talk about their work.”
Kathleen Collins has been producing Indoor Voices since the summer of 2017. She started the podcast as “a way to highlight the fascinating things going on around CUNY that might not be widely known. There are so many inhabitants in the CUNYverse doing incredibly interesting things… We like being able to provide a low-stakes, easy-to-share platform for people to talk about their work.”
To Kathleen, the conversations are the key element. She and her co-host, La Guardia Community College librarian Steven Ovadia, interview CUNY faculty, students, alumni and staff members about their research or creative output; they have a great deal of leeway to highlight what interests them.
 Nick Rodrigo is new to podcasting, overcoming challenges as he meets them in the course of creating They Are Just Deportees. The newly-launched show examines the various ways in which the U.S. immigration enforcement system shapes and controls the lives of migrant communities in this country. With co-host Darializa Avila Chevalier, TAJD helps listeners to understand “the multiple sites of border enforcement in the U.S., and the punitive effects of the country’s periodic moral panics on the ‘criminal alien.'”
Nick Rodrigo is new to podcasting, overcoming challenges as he meets them in the course of creating They Are Just Deportees. The newly-launched show examines the various ways in which the U.S. immigration enforcement system shapes and controls the lives of migrant communities in this country. With co-host Darializa Avila Chevalier, TAJD helps listeners to understand “the multiple sites of border enforcement in the U.S., and the punitive effects of the country’s periodic moral panics on the ‘criminal alien.'”
Nick, and his associates in the Social Anatomy of a Deportation Regime Working Group (the sponsor of the podcast), think this is a particularly relevant topic. “Immigrant rights have come under increasing threat from the state, with bans on immigration from Muslim majority countries, the detention of children at the U.S./Mexico border, and the pledge of this administration to increase the forced removal of all undocumented people. … It is vitally important that the deportation system — which expels up to 300,000 persons a year — be placed in the historical context of this country’s treatment of the ‘other,’ while focusing on the real time implications of the current system on immigrant communities.”
For both showrunners, podcasting is a great way to make sometimes-complex issues and scholarship more accessible to an average listener. Says Nick, “two of the major issues in scholarship today are the ‘ivory tower’ mentality of academics and a lack of interdisciplinary focus on major social issues. Conferences and public lectures can be delivered in such inaccessible language that they can be alienating to non-academics. Podcasting allows for the complex issues concerning immigration enforcement to be distilled and presented to the public in a way that is accessible and digestible, with the opportunity for the listener to pause, reflect, and reengage at their own pace. Podcasting also provides a platform for criminologists, sociologists, public health experts, geographers, and journalists to come together on an issue and, if the interview structure is good, a compelling narrative for change can be constructed.”

Kathleen also wants to make it easier for non-experts to engage with what CUNY produces. “There is so much going on within CUNY,” she says, “and it shouldn’t be hidden inside the academy. Podcasts are a good way to get people interested in new things — it’s a mini, portable seminar for your ears. But since Steve and I act as generalists in our role as interviewers, we can hopefully elicit a layman’s interpretation of what scholars are thinking and writing about. The point is to bring attention to the author or artist, and ask about their research and writing process and teaching — these topics bring the conversation to a universal level.”
Creating content to fit the platform can sometimes be challenging. Nick was “forced to learn new skills on the job,” but found that his struggles with editing gradually turned into confidence! Kathleen cites the extensive support and inspiration from other podcasters and staff at the college as a source of her success and joy in creating Indoor Voices.
In the end, she says she loves every episode she produces — thanks to the satisfying conversations and intimate connections she can form with guests during a 40 minute interview, each new episode supplants the last as her new favorite.
Check out the latest episodes of Indoor Voices, They Are Just Deportees, and more John Jay podcasts:
- Indoor Voices: J Journal founders Adam Berlin and Jeffrey Heiman have been producing the literary magazine for twelve years. The high quality creative work they feature deals with contemporary justice issues, but not always in a way you might expect.
- They Are Just Deportees: You can find the first six episodes on the Social Anatomy of a Deportation Regime website, or by searching on Spotify.
- Reentry Radio: The latest episode of the podcast produced by John Jay’s Prisoner Reentry Institute deals with employment discrimination against justice-involved individuals, with special guest Melissa Ader of the Legal Aid Society’s Worker Justice Project.
- This World of Humans: Host Nathan Lents talks to Hunter College researcher Dr. Jill Bargonetti about using mouse models to study triple-negative breast cancer.
Policies Changing New York: Impact Magazine 2018-19

As a New York institution and part of the City University of New York, John Jay College is home to many who want to drive real-world reform to make New York communities stronger. Our unique research centers provide evidence-based partnerships and guidance that city officials and state legislators need to create better policy. Read on for a quick look at the impactful work they are doing in New York, or read the full story in our latest issue of Impact research magazine.
Easing Reentry
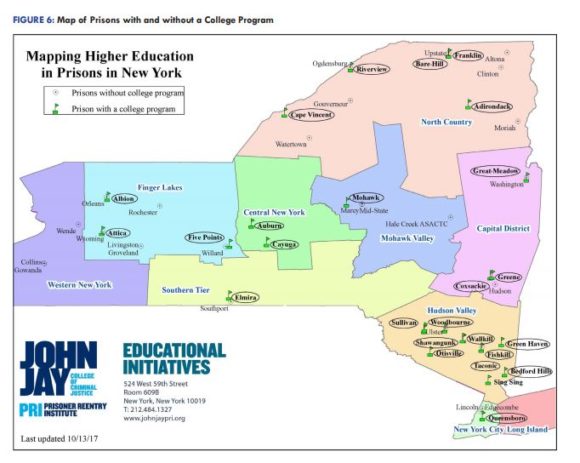
The Prisoner Reentry Institute has been a research center since 2005, when it was founded to help people live successfully in their communities after contact with the criminal justice system. The center, directed by Ann Jacobs, engages in a combination of public advocacy, direct service, and collaborative partnerships to promote a range of reentry practices, with a focus on creating pathways from justice involvement to education and career advancement.
In pursuit of that goal, PRI advocates for higher education in prisons, priming what they call the “prison-to-college pipeline.” They recently produced a report mapping higher education opportunities in New York State prisons, finding that only 3% of more than 45,000 people in New York prisons were participating in higher education programs, despite expanded funding.
PRI is also interested in post-incarceration advocacy. A work group, led by PRI’s Director of Public Policy Alison Wilkey and comprised of local stakeholders, is working to change the New York City Housing Authority’s policies excluding residents who have been arrested. The work group’s actions, including the creation of a clearer exemption application, new guidelines limiting the use of exclusions, and tenant education, have helped reduce the number of people excluded from NYCHA housing 50% from 2016 to 2018.
Interrupting Crime

A team of Research and Evaluation Center researchers is evaluating Cure Violence, a public health approach to violence reduction.The program relies on neighborhood-based workers, often with a history of justice involvement, mediating and working with younger people in the neighborhood to keep them from going down a violent path.
“Politically, it’s a difficult program to operate,” says REC Director Jeff Butts, because city officials are often wary of Cure Violence workers’ criminal histories. But REC has found that Cure Violence sites in the South Bronx and Brooklyn have seen greater violence reductions than comparison sites. According to Butts, explaining the research and the results clearly to the public is key to shifting policy. “You can’t change policy, no matter how smart you are, just by publishing articles in academic journals.”
Less Punishment, Less Crime
Violence isn’t the only type of crime that can be reduced with less punitive solutions. Director of research project From Punishment to Public Health (P2PH) Jeff Coots holds that alternatives to incarceration can not only reduce the use of prison and jail terms, but also offer rehabilitative services to people in need. “Punishment alone is not getting us the public safety outcomes we want,” he says. “How do we identify public health-style solutions that can respond where punishment does not, and isolation will not?”
Among P2PH’s signature initiatives is a pilot project to use pre-arrest diversion for minor offenses committed by the homeless. Many of those cases were previously decided at arraignment, denying arrestees the chance to connect with needed services. The pilot has reduced the number of people arrested and increased the number connected with services like transitional housing and health treatment.
In general, Coots believes policymakers are increasingly open to health interventions as an alternative to incarceration. “We don’t want the jail to be the biggest mental health provider in our community.”
Justice by the Numbers
The Data Collaborative for Justice is invested in documenting the scale of the criminal justice footprint, in New York and a network of other cities, and

considering solutions to reduce it. DCJ explores high-contact points in the system, including pretrial detention and incarceration in New York City jails. A major project for the center has been to produce an evaluation of the 2016 Criminal Justice Reform Act, passed by the New York City Council to “create more proportional penalties for certain low-level, nonviolent offenses.” With support from the Mayor’s Office of Criminal Justice, DCJ’s evaluation shows that the CJRA seems to be achieving its aims — 90% of summonses for five high-volume offenses like noise violations and littering are now civil rather than criminal, with an associated decline in criminal warrants.
The positive impact of this legislation has the potential to push policy change in other areas by informing conversations with lawmakers. DCJ works closely with city and state agencies to gather data and make it available to policymakers so they have the resources to make evidence-based decisions. “Policy neutrality is an important part of DCJ’s mission and outlook,” says Project Director Kerry Mulligan. “That has allowed us to be a trusted broker with a diverse set of data partners.”
Among John Jay College’s research centers and projects, some researchers are building the evidence base, while others are rolling up their sleeves to help cities implement and evaluate solutions on the ground. In each case, the vital goal is making communities safer. Says REC’s Jeff Butts, “You have to put the evidence in front of [policymakers] on a regular basis in order to get the political culture to start to shift.”
For the full feature, please visit the John Jay Faculty and Staff Research page to read the whole magazine in PDF form!
John Jay Scholars on the News – Vaccines and the Flu
It’s winter, which we sometimes call “flu season.” In fact, “you can catch influenza at any time during the year if exposed to the virus, and its severity is the same regardless of when you get sick,” says Edgardo Sanabria-Valentín. We don’t fully know the answer to why influenza is more common during the colder months. According to Nathan Lents, “The virus is viable for a longer time in cold air, and spreads more readily in dry air. Another reason that may contribute is that winter air dries our mucus membranes, which makes them less effective at preventing viral entry. We also tend to spend more time indoors with closed windows and recirculated air.”
A somber anniversary

The 2018 flu season was also the 100th anniversary of the infamous global influenza pandemic, a year when more
than 500 million people around the world are estimated to have died from flu. Of that number, 675,000 fatalities came from the United States, with roughly 20,000 from New York City alone. According to Mike Wallace, in his 2018 book Greater Gotham, more Gothamites died of disease in the city than died during World War I; the ongoing war effort actually impaired New York’s efforts to fight the flu, by concentrating soldiers in training camps where disease could spread and by taking much-needed medical personnel away from home to establish medical camps near the battlefields in Europe.
Despite the high numbers of fatalities at home, New York of 1918 had a lower death rate than other major cities (4.7 deaths per 1,000 residents, as compared to Boston’s rate of 6.5 and Philadelphia’s of 7.3). This was attributed by Health Commissioner Royal Copeland to New York’s long history of public health work, and particularly the alleviation of unhealthy conditions around the city at the turn of the 20th century.
Vaccines and you

Today, scientific and public health efforts have brought some protection from a repeat of 1918 in the form of vaccines. In the case of the flu, explains Dr. Lents, “Each year’s vaccine is targeted toward the three to four strains that appear to be spreading the most rapidly. The injected vaccine contains killed viruses [from those strains], while the nasal spray contains live but weakened viruses. In both cases, the large dose of viral particles elicits a strong immune reaction from our bodies, including the production of antibodies that can stick around for years or even decades. The second time we are exposed to the same virus, it only takes a day or two to mount the same level of immune response. This ‘priming’ gives the immune system enough of a head start that it usually prevents the infection from ever taking hold.”
Because the influenza virus is so good at mutating from year to year, “no vaccine is 100% perfect, and getting the flu shot will never protect you against 100% of all flu strains,” says Dr. Sanabria-Valentín. But the vaccine will “significantly decrease the risk of getting sick, and will decrease the severity and length of infection, and decrease the chance that you get other people sick” if you do contract the virus.
Vaccinating also helps to protect those around you in other ways, namely by contributing to “herd immunity.” “Some people cannot be vaccinated because they are too young, too old, immune-compromised, or battling other kinds of infections,” says Dr. Lents. When the percentage of people in a population are effectively immunized, it helps to prevent the spread of disease to those who were unable to receive the vaccine. But when the percentage of vaccinated people falls because individuals who otherwise could be immunized choose not to be, it puts vulnerable populations at risk.
Conquering vaccine hesitancy

“Controversies about vaccinations have been out there since we adopted this preventative measure almost 100 years ago,” says Dr. Sanabria-Valentín. “There are a lot of myths about vaccinations which are peddled by conspiracy theorists trying to sell you something or by people who might have good intentions but got swindled by ill-intentioned people trying to make a fast buck. One of the most popular ones is that vaccines can cause autism in children. This claim was first made in a study that was demonstrated (by many groups) to be fraudulent; no direct relationship between receiving vaccinations and autism has been found. There is overwhelming consensus among scientists and physicians that vaccines are safe and effective even though, like most medical treatments, in very rare cases they can cause side effects and in even rarer instances can cause serious unintended health problems. There is overwhelming evidence that vaccination has helped not just individuals, but humankind.” Although diseases like smallpox, polio and the measles were all but eliminated by vaccine technology, skepticism about immunization–which many attribute to the rise of social media–has caused some long-gone diseases to stage a comeback.
Dr. Lents stated that “in 2017, 80,000 people died of influenza, the highest number in 40 years. If more healthy people had been vaccinated, that number could have been much less. Each person that decides not to vaccinate adds a little bit of risk to the entire population.” This dynamic played out in October 2018, when measles–which was declared eliminated in the US in 2000–broke out in Williamsburg, Brooklyn. The New York City Department of Health confirmed 42 cases in Williamsburg and Bensonhurst as of mid-December, and is currently barring un-immunized students from attending local schools. And according to The Guardian, Europe is also experiencing a surge in vaccine hesitancy and a corresponding growth in the numbers of new measles cases; Europe will see more than 60,000 new cases this year and 72 deaths, the highest number this century.

It is generally agreed that fears about vaccine side-effects are overblown, and contradicted by scientific consensus. “Vaccines are constantly monitored and modified as circumstances dictate. The FDA does not approve a vaccine unless initial trials indicate the benefits clearly outweigh the risks. In response to vaccine safety concerns today, healthcare providers have to give vaccine information sheets to recipients clearly describing the risks and benefits of the vaccine. And finally, vaccines are subject to particularly high safety standards because, unlike other health treatments, they are given as preventive measures to protect healthy people,” explains Dr. Evelyn Aranda Jaque. “Although vaccination is not 100% effective, studies on flu vaccination programs have shown that people who get vaccinated are less likely to be seriously ill or die in comparison with those who do not vaccinate. We must consider that the widespread use of vaccines for life-threatening diseases in the United States has led to a dramatic decrease in their incidence.”
Evelyn Aranda Jaque is a substitute Associate Professor at John Jay College, where she teaches classes including Immunology and Microbiology. She received her Ph.D. from the Physiology Department at Pontificia Universidad Católica de Chile. Dr. Aranda Jaque’s research since her doctorate days has largely focused on the role of angiogenesis (the formation of new blood vessels) in tumor progression.
Nathan Lents is a Professor of Biology and Director of the Honors Program and Macaulay Honors College at John Jay College. He holds a Ph.D. in human physiology and postdoctoral training in computational biology from NYU. In addition to his laboratory research, Dr. Lents writes popular science articles, blog and books. His most recent book is Human Errors: A Panorama of Our Glitches from Pointless Bones to Broken Genes.
Edgardo Sanabria-Valentín is the Associate Program Director of John Jay College’s Program for Research Initiatives in Science and Math (PRISM) as well as the college’s Pre-Health Careers Advisor. He holds a Ph.D. from NYU-School of Medicine, and spent three years working in the biotechnology industry. Dr. Sanabria-Valentín is the recipient of the ESCMID Young Scientist Award (2007), a Leadership-Alliance Schering Plough Graduate Fellowship (2006), and the NBHS-Frank G. Brooks Award for Excellence in Student Research (2001).
Mike Wallace is a Distinguished Professor of History at John Jay College and author of Greater Gotham: A History of New York City from 1898 to 1919. Dr. Wallace is also the co-author of Pulitzer Prize-winning Gotham: A History of New York City to 1898 and the founder of the Gotham Center for New York City History at the CUNY Graduate School. He received his undergraduate and graduate degrees from Columbia University.
John Jay Scholars on the News – The Opioid Epidemic
The terms “opioid crisis” or “opioid epidemic” have come to be used as political buzzwords, but what does it really mean to say that America is in the grip of an “opioid epidemic”? According to the Centers for Disease Control, more than 72,000 people in the United States died as the result of an overdose in 2017, and approximately 30,000 of these were from the use of fentanyl and other synthetic opioids — that comes to around 100 per day! Fentanyl, a powerful opioid designed to treat severe and chronic pain, is roughly 100 times stronger than morphine, and is currently being used to adulterate other abused substances, making these overdoses likely to increase.
From the perspectives of policy, policing, and public health, this rash of deaths is worthy of further consideration. John Jay College scholars from across disciplines and research areas tell us what they think has contributed to the trend of deaths from opioid abuse and what approaches may be best suited to tackling the problem.
What is different about the pattern of drug abuse we are seeing today that has caused it to be referred to as the “opioid epidemic”?
Jeff Coots (Director, From Punishment to Public Health Initiative): One main reason for concern around opioids today is that they are simply more deadly than the other drugs we consume. However, the rates of overall illicit drug use are actually quite steady — especially when we remove cannabis consumption from the conversation. The latest results from the National Survey on Drug Use and Health show steady illicit drug consumption from 2002-2013 at about 4%, with those aged 18-25 using a bit more than twice the rate of other age groups. We do see a slight increase in heroin consumption as prescription opioids become less available, but this doesn’t impact the overall rates of illicit consumption.
Heidi Hoefinger (Visiting Scholar, Anthropology): The situation is considered an “opioid epidemic” due to the size of the problem now, and its potential for growth. But this issue is also getting more attention than past drug “epidemics” because it’s a white, middle-class problem, particularly here in New York, with Staten Island and Long Island having some of the highest rates of use and overdose. There has definitely been a “softer” approach to this epidemic as opposed to the “crack epidemic” of the 1980s, which saw much more aggressive law and order efforts resulting in mass incarceration. Many poor people of color are still sitting in prison because of that heavy-handed approach. It’s definitely a good thing that opioid addiction is currently being viewed as more of a public health issue, but it’s extremely problematic that Black and Latinx folks continue to suffer the consequences of racist applications of drug policy.
Can you point to a few of the key factors that you believe are to blame for the current public health crisis?
Jeff: The origins of the current crisis began with the marketing of OxyContin as a non-addictive painkiller in the 1990s followed by the introduction of “pain” as the fifth vital sign in 2001. This led to higher rates of opioid prescription drug use and related overdose fatalities in the early 2000s. The second “wave” of opioid-related deaths are attributed to increased heroin consumption starting in about 2010, following a crackdown on prescription opioid distribution — consumers simply switched to the cheaper and more available opioid. The third wave is attributed to the increased presence of synthetic opioids like fentanyl in the market, starting in about 2013. These synthetics can be much more potent and make it difficult for users to control their dosage, leading to more overdoses.
Marta Concheiro-Guisan (Assistant Professor, Forensic Toxicology): Other socioeconomic factors like unemployment and economically-depressed areas should also be considered in trying to understand the whole problem and the populations most affected by it.
Heidi: The biggest drivers are probably Big Pharma and corporate greed because pharmaceutical companies were deceptive about the true effects of opioids, claiming they were non-habit inducing. They also offered incentives to doctors for prescribing, which led doctors to over-prescribe opioids instead of safer alternatives. Insurance companies typically cover opioids as opposed to alternative therapies, so they’ve played a role in this as well. It’s encouraging to see that NYC (among other cities) is suing some major pharmaceutical companies for their role in the epidemic, but there still needs to be more accountability on the part of Big Pharma.
What are the implications for American society should this systemic issue continue unabated?
Jeff: I think we are having a really important debate in the country right now about how our collective response to drug use differs along racial lines. Drug Policy Alliance and Columbia University co-hosted a conference in 2016 to highlight how the white opioid user who may have started on prescription drugs and then switched to heroin is considered a victim of circumstance and provided overdose treatment, rehabilitation and a call for compassionate public health responses. Meanwhile, black and brown heroin addicts who may not have had health insurance and access to prescription drugs tend to get jail cells, court-mandated treatment and moralizing “just say no” campaigns grounded in personal responsibility. Obviously, the the shift towards funding treatment and reducing criminal justice involvement is welcome, but the carnage reaped in the previous regime of zero tolerance and deterrence must be acknowledged and reconciled at the local and national levels.
Heidi: It has been compared to HIV in some arenas, in that it’s affecting a marginalized and stigmatized population (e.g., drug users) but it’s not getting the same attention and funding it deserves. The numbers of overdoses and deaths will likely continue to rise as long as the stigma exists, and as long as pharmaceutical companies continue to operate unchecked, as long as doctors continue over-prescribing, as long as insurance companies don’t see the value in covering alternative treatments, and as long as harm reduction remains undervalued and underfunded.
Marta: The biggest impact on American society is, of course, the tragedy of the families affected by this unprecedented health issue, and the loss of so many young people’s lives. The Centers for Disease Control and Prevention estimates that the total “economic burden” of current opioid misuse alone in the United States is $78.5 billion per year, including the costs of healthcare, lost productivity, addiction treatment, and criminal justice involvement.
 The Opioid Crisis Response Act of 2018 was recently signed into law. It authorizes new funding and grants to address the crisis, advances initiatives to raise awareness and to get more first responders to carry naloxone, and drives increased coordination among federal agencies to stop drugs like fentanyl at the border, among other measures. Do you think this bill takes the right approach to dealing with the crisis? Does it go far enough?
The Opioid Crisis Response Act of 2018 was recently signed into law. It authorizes new funding and grants to address the crisis, advances initiatives to raise awareness and to get more first responders to carry naloxone, and drives increased coordination among federal agencies to stop drugs like fentanyl at the border, among other measures. Do you think this bill takes the right approach to dealing with the crisis? Does it go far enough?
Heidi: Many of these are welcome changes, and are actually similar to Obama’s opioid plan from 2016, but the problem is that this plan doesn’t allocate much more funding — which is needed. If this is a serious public health problem, it should receive funding and attention similar to that provided for HIV/AIDS or Ebola, as well as a similarly concerted, multi-organizational response. But addiction is still a very stigmatized condition, and not taken as seriously as it should be. People with addictions are still often blamed for their own demise, and not viewed in the same light as people with other chronic illnesses.
Marta: From my point of view, one critical element in addressing this crisis is the treatment of addiction as a health issue rather than as a stigma, and a drastic improvement of current services and their accessibility. Another important aspect is education for the general population and among professionals such as medical doctors. More funds are also necessary for the forensic sciences to develop a clearer picture of the current crisis, to know all the opioids that are involved, to monitor future crises, and to research addiction.
Jeff: We need to invest heavily in reducing demand and mitigating the risks associated with consumption, rather than focus on interrupting supply. Efforts to control access to drugs have failed for over a century. In reducing demand, we need to do a better job of addressing pain and trauma, take a hard look at our overreliance on pharmaceuticals and reduce the number of people who become addicted in the first place. In working with those already experiencing opioid dependence, we need to provide competent and evidence-based care including Medication Assisted Treatment (MAT), which is the gold standard for treating those with opioid disorders. In terms of mitigating risks, increased naloxone access is crucial, but increased use of other Harm Reduction strategies is needed as well.
What do you believe is the best way to address this epidemic?
Marta: This epidemic has to be addressed with a multidisciplinary approach, as indicated by the National Institute on Drug Abuse (NIDA) and other governmental agencies. Promoting the use of naloxone, the improvement in the accessibility of medical assistance and addiction treatments, the expansion of prevention programs in schools and for the general public, and increasing funds for the forensic sciences and addiction research are among what I consider the priority areas.
Jeff: The best way to reduce the impact of opioid overdose fatalities is to focus on saving the lives of those who choose to consume opioids. This strategy, more commonly known as Harm Reduction, focuses on reducing the negative side effects associated with illicit drug use, rather than punishing and/or moralizing at those who engage in use. These strategies include needle exchange programs, peer-based education, MAT programs, and safe consumption facilities, all of which treat those who consume illicit drugs as human beings worthy of compassion and competent medical care for their medical issues. As I noted earlier, our previous strategy of interrupting supply and punishing consumption — i.e., the War on Drugs — has not reduced the rates at which our citizens consume illicit drugs. It has, however, made that consumption more dangerous and more damaging for those communities with higher rates of use and criminal justice presence.
Heidi: Societal attitudes towards drug users and people with addictions need to change. For this to happen, people need to understand that drug use has always been a part of human history, drug users are not inherently bad people, and people will continue to want to alter their consciousness or treat pain through drug use. People also need to understand the racialized history of drug policy in this country, and that laws against drug use (which are unevenly applied across race and class) were implemented for racial, class and economic reasons (and because of who was using the drugs), not necessarily because of the harmful effects of the drugs. When people are exposed to this history, and these realities, then perhaps stigma against drug use will change, and people affected by the current epidemic will get the proper help that they need.
In addition, we need more funding for harm reduction and evidence-based drug education programs in middle schools, high schools, college and universities. Not the “Just Say No” type, because those don’t work. But the kind where students can ask open, honest questions and get factual, evidence-based, non-biased, non-moralistic responses so they can know the potential effects and risks and make more informed decisions. And there also needs to be more support for medication-assisted treatment programs (like methadone and buprenorphine), as well as harm reduction programs like DanceSafeNYC that provides factual, evidence-based drug education and drug checking kits at music festivals and events. These types of initiatives take harm reduction beyond syringe exchange programs and make them more accessible to a diverse range of young people, which ultimately saves lives, and may start to turn the tide of this epidemic.

Marta Concheiro-Guisan, Ph.D., is Assistant Professor of Forensic Toxicology at John Jay College. She has experience in the development and validation of new analytical methods and toxicological analysis of different types of specimens–including plasma, blood, urine, oral fluid, hair, sweat and other tissues. She has participated in Drugs and Driving Research Projects, including the ROSITA (Road Site Testing Assessment) and DRUID (Driving Under the Influence of Drugs) European Projects, to study alternative matrices to detect drug impairment, and in clinical protocols involving different types of drugs of abuse and drug exposure during pregnancy. Dr. Concheiro-Guisan has more than 40 publications in peer-reviewed journals.
 Jeff Coots, JD, MPH, serves as the Director of the From Punishment to Public Health (P2PH) initiative based at John Jay College. Prior to joining P2PH, Mr. Coots completed a joint Juris Doctor/Masters of Public Health degree program at Northeastern University School of Law and Tufts University School of Medicine, where he focused his studies on the social justice and health impacts of mass incarceration. While in Boston, he served as an Albert Schweitzer Fellow and delivered dialogue-based “Health Reentry” workshops to introduce strategies for working in collaboration with a primary care provider to prevent new infections and mitigate the effects of chronic disease.
Jeff Coots, JD, MPH, serves as the Director of the From Punishment to Public Health (P2PH) initiative based at John Jay College. Prior to joining P2PH, Mr. Coots completed a joint Juris Doctor/Masters of Public Health degree program at Northeastern University School of Law and Tufts University School of Medicine, where he focused his studies on the social justice and health impacts of mass incarceration. While in Boston, he served as an Albert Schweitzer Fellow and delivered dialogue-based “Health Reentry” workshops to introduce strategies for working in collaboration with a primary care provider to prevent new infections and mitigate the effects of chronic disease.
 Heidi Hoefinger, Ph.D., is a Visiting Scholar in John Jay College’s anthropology department, where she teaches a course on gender and sexuality within the social and cultural contexts that exist in an increasingly integrated but unequal global world. She also works on a large European Research Council (ERC) project led by Kingston University in London, in which she is the New York-based ethnographer looking at anti-trafficking efforts in New York City, and their effect on sex work/ers and migration policy. Among her areas of interdisciplinary research interest are gender and sexuality, globalism and transnationalism, and drug use.
Heidi Hoefinger, Ph.D., is a Visiting Scholar in John Jay College’s anthropology department, where she teaches a course on gender and sexuality within the social and cultural contexts that exist in an increasingly integrated but unequal global world. She also works on a large European Research Council (ERC) project led by Kingston University in London, in which she is the New York-based ethnographer looking at anti-trafficking efforts in New York City, and their effect on sex work/ers and migration policy. Among her areas of interdisciplinary research interest are gender and sexuality, globalism and transnationalism, and drug use.
National Network for Safe Communities Hosts Film Screening, Panel on Opioid Crisis

By Raymond Legendre
Amidst the deadliest drug epidemic in American history, the National Network for Safe Communities (NNSC) hosted a documentary film screening and panel discussion on October 2 that highlighted why the opioid crisis is so difficult to stop, and shared the actions being taken in New York City to save lives.
The event featured the Mother Jones short documentary series, Finding a Fix, with a brief introduction by filmmaker Mark Helenowski, and a subsequent panel conversation including New York City council member Stephen Levin, Manhattan Assistant District Attorney Kaitrin Roberts, and community organizer Marilyn Reyes, co-chair of the Peer Network of New York. Mother Jones reporter Julia Lurie also participated on the panel, which was moderated by NNSC Director David Kennedy.

In 2017, drug overdoses claimed an estimated 72,000 lives in the U.S., according to the Centers for Disease Control and Prevention. Of those deaths, more than 49,000 were attributed to opioids. New York City alone recorded around 1,500 overdose deaths last year. The current death rate is equal to one New Yorker dying from an overdose every six hours, according to ADA Roberts. The availability of Narcan, a nasal spray that can reverse opioid overdose, is often the different between fatal and non-fatal overdoses, the prosecutor also noted. In August 2017, New York became the first state to make no-cost or lower-cost medicine to reverse opioid overdoses available at pharmacies.
To learn more about the event, read the rest of this article on the NNSC website. To learn more about the work NNSC does, visit their homepage.
 Eric Piza is an Associate Professor of Criminal Justice at John Jay College of Criminal Justice. His research focuses on the spatial analysis of crime patterns, problem-oriented policing, crime control technology, and the integration of academic research and police practice. His recent research has appeared in peer-reviewed journals including Criminology, Criminology & Public Policy, Crime & Delinquency, Journal of Quantitative Criminology, Justice Quarterly and more. In support of his research, Dr. Piza has secured over $2.2 million in outside research grants, including funding from the National Institute of Justice. In 2017, he was the recipient of the American Society of Criminology, Division of Policing’s Early Career Award in recognition of outstanding scholarly contributions to the field of policing.
Eric Piza is an Associate Professor of Criminal Justice at John Jay College of Criminal Justice. His research focuses on the spatial analysis of crime patterns, problem-oriented policing, crime control technology, and the integration of academic research and police practice. His recent research has appeared in peer-reviewed journals including Criminology, Criminology & Public Policy, Crime & Delinquency, Journal of Quantitative Criminology, Justice Quarterly and more. In support of his research, Dr. Piza has secured over $2.2 million in outside research grants, including funding from the National Institute of Justice. In 2017, he was the recipient of the American Society of Criminology, Division of Policing’s Early Career Award in recognition of outstanding scholarly contributions to the field of policing.


Recent Comments